How Your Microbiome Influences Your Metabolism, Mood, and Mind.
How Your Microbiome Influences Your Metabolism, Mood, and Mind
Last month we looked at gut inflammation what drives it, how to identify it, and why it matters. This month, we're building on that foundation. Inflammation doesn't exist in isolation. It is one of the key mechanisms through which a disrupted microbiome affects systems far beyond the gut your metabolic health, your neurological function, and your mental wellbeing.
Your microbiome is not a passive digestive bystander. It is an endocrine, immune, and neurological organ and understanding how it functions gives you a significant clinical advantage.
The microbiome and metabolic health
When beneficial bacteria, particularly (Akkermansia muciniphila, Faecalibacterium prausnitzii, and Bifidobacterium species) ferment dietary fibre, they produce short-chain fatty acids (SCFAs): butyrate, propionate, and acetate. Each has a distinct metabolic role:
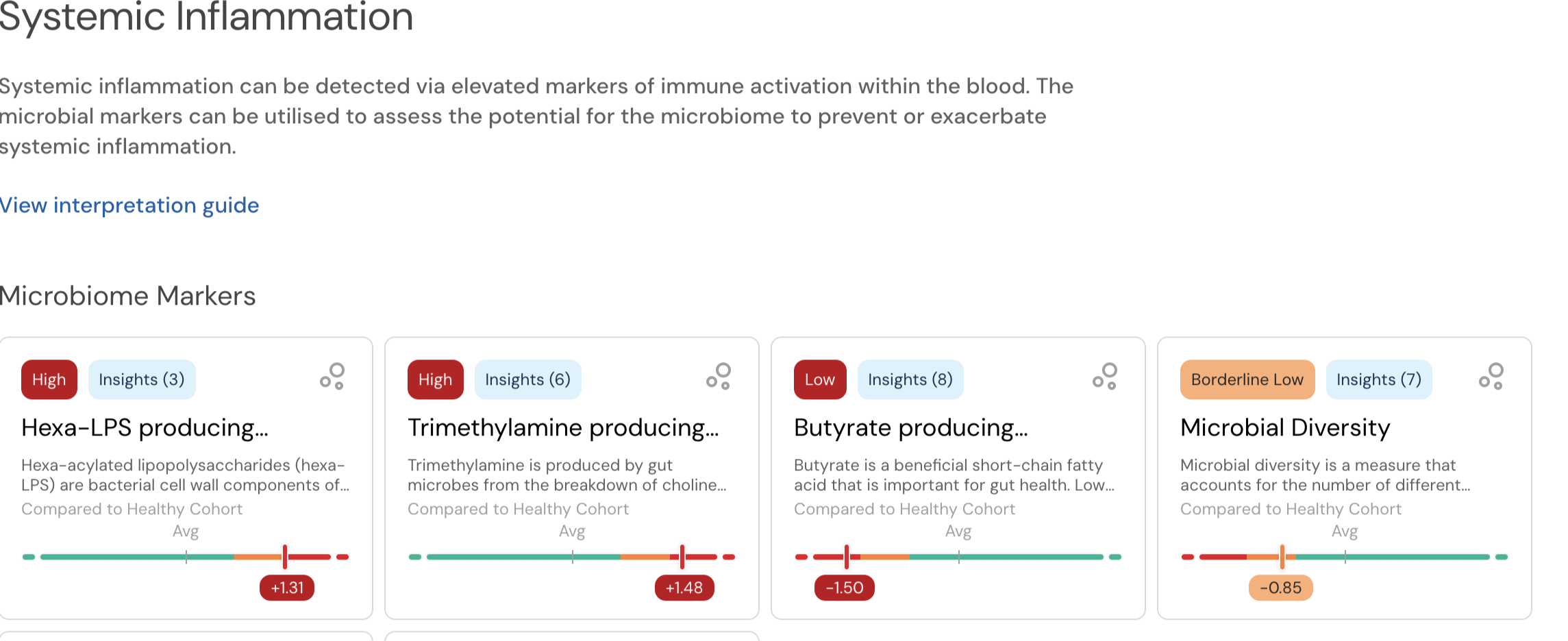
Butyrate fuels colonocytes, maintains gut barrier integrity, and regulates inflammatory gene expression.
Propionate modulates hepatic gluconeogenesis and supports insulin signalling
Propionate and acetate together stimulate appetite-regulating hormones
When microbial diversity declines, through low-fibre intake, antibiotic exposure, or chronic stress SCFA production is compromised. Bacterial lipopolysaccharides (LPS) translocate into systemic circulation, insulin signalling is impaired, and low-grade chronic inflammation takes hold.
Clinically, this presents across a range of conditions:
Insulin resistance and type 2 diabetes — dysbiosis is now considered a contributing mechanism.
PCOS — reduced Lactobacillus and elevated inflammatory species drive androgen dysregulation and insulin resistance
NAFLD — LPS translocation through a compromised gut barrier promotes hepatic inflammation
Hashimoto's thyroiditis — dysbiosis impairs peripheral T4 to T3 conversion, with gut permeability increasingly linked to autoimmune thyroid activity
What this looks like on a CoBlome gut test
A Microba CoBiome gut test provides detailed metagenomic analysis of your microbial ecosystem identifying which species are present, at what abundance, and how they compare to a healthy reference population. Clinically, this moves us beyond symptom management to identify specific microbial drivers behind metabolic dysfunction, inflammation, or immune dysregulation.
A result might reveal depleted Akkermansia muciniphila, a keystone species associated with gut barrier integrity and insulin sensitivity or reduced SCFA-producing bacteria overall, explaining persistent fatigue, blood sugar instability, or weight management difficulty despite a reasonable diet.
The microbiome and the brain
The gut-brain connection is bidirectional, continuous, and clinically underestimated. Your enteric nervous system contains approximately 500 million neurons. Around 95% of your body's serotonin is produced in the gut cells, with the microbiome playing a significant role in regulating how much is actually synthesised. Communication occurs via the vagus nerve, the HPA axis, and immune signalling pathways.
Specific species have demonstrated measurable neurological effects:
Lactobacillus rhamnosus reduces anxiety behaviours and may affect GABA
Bifidobacterium longum modulates cortisol reactivity and stress response
Tryptophan - the serotonin precursor is also microbiome regulated. In dysbiosis, can reduce serotonin availability and increasing neuroinflammatory metabolites.
Symptoms often present as psychological but have a clear physiological driver persistent low mood, cognitive fatigue, heightened stress reactivity, disrupted sleep, and IBS that doesn't resolve with dietary intervention alone.
How they reinforce each other
Gut dysbiosis drives systemic inflammation, activating the HPA axis and elevating cortisol. Chronically elevated cortisol impairs insulin sensitivity and promotes visceral adiposity. Disrupted serotonin signalling compromises sleep, which further reduces insulin sensitivity and elevates ghrelin. Stress then shifts microbial composition toward pro-inflammatory species and the cycle continues.
Addressing the gut can be an effective entry point for conditions that appear metabolic, neurological, or hormonal in origin.
Microbiome and metabolic health:
Aim for 30 different plant foods per week — fibre diversity drives microbial diversity
Prioritise prebiotic-rich foods: Jerusalem artichoke, green banana, cooked and cooled potato (resistant starch), leek, and chicory
Include polyphenol-rich foods daily — blueberries, extra virgin olive oil, green tea, dark chocolate (85%+)
Eat oily fish two to three times per week for omega-3s that reduce intestinal inflammation and improve insulin sensitivity
Swap refined carbohydrates for low-glycaemic alternatives — legumes, lentils, oats, sourdough, basmati rice and pair carbohydrates with protein, fat, or fibre
Eat within a consistent 10 - 12 hour window (e.g. 8am–6pm) to support circadian alignment and improve fasting insulin
Chew thoroughly and eat slowly - gastric acid and digestive enzyme output directly affect microbial composition.
Limit alcohol - even moderate intake disrupts the gut mucosal barrier and reduces Lactobacillus and Bifidobacterium abundance
Hydration — adequate water intake supports mucosal integrity and short-chain fatty acid transport
Gut-brain axis:
Include fermented foods daily - kefir, kimchi, sauerkraut, or live culture yoghurt
Regulate stress consistently — 10 minutes of diaphragmatic breathing activates the vagus nerve and shifts autonomic balance
Protect sleep — even short-term disruption alters microbial composition and reduces insulin sensitivity within days
Fun and Play - these are not indulgences but evidence-based vagal tone stimulators that directly shift your autonomic nervous system toward parasympathetic dominance.
Spend time in natural environments - exposure to environmental microbiota through soil, plants, and outdoor air increases microbial diversity and has demonstrated reductions in cortisol and inflammatory markers
Limit ultra-processed foods - beyond sugar and refined carbs, emulsifiers and artificial additives have been shown to directly disrupt the gut mucosal layer and alter microbial composition independently of macronutrient content
Targeted supplementation and clinical interventions require individual assessment.
Working with me
I use detailed case history, comprehensive blood pathology, and functional gut testing to identify specific drivers, not generalised protocols. This will include alongside Microba CoBlome gut testing, and exploration of inflammatory markers, fasting insulin, HbA1c, thyroid function, and nutrient status will provide a whole person picture of your metabolic and microbial health.
Not sure where to start? A discovery call is the place to begin.
For those focused on prevention, identifying microbial imbalance or insulin dysregulation before symptoms develop allows for intervention when outcomes are significantly better. Prevention is not a passive strategy. It is the most evidence-based one available.